Vaccination decisions are usually quite simple. People may or may not meet criteria for vaccines based on their age or other factors. But when a federal panel recently recommended an update of human papillomavirus (HPV) vaccine guidelines, it left a lot of uncertainty.
The panel recommended that men and women aged 27 to 45 decide, in conversation with their doctors, whether it made sense for them to be vaccinated against HPV.
But some public health advocates criticize that advice because they say it doesn’t provide doctors and patients with clear guidance about who are good candidates in this broad age group. They are also concerned that many people will get vaccinated and not benefit, adding unnecessary costs to the system and possibly reducing the number of people who could get vaccinated abroad, where HPV vaccine is in short supply.
“My concern is that there will be a lot of people or doctors recommending this vaccine,” said Debbie Saslow, managing director of HPV and gynecologic cancers for the American Cancer Society. “But I think the benefit is very small and we just don’t have guidance.
Human papillomavirus is the most common sexually transmitted infection in the United States; almost everyone who is sexually active will get it at some point. People usually clear the virus themselves and often don’t even realize they were infected. But in some people, HPV remains in the body and can cause several types of cancer, as well as genital warts.
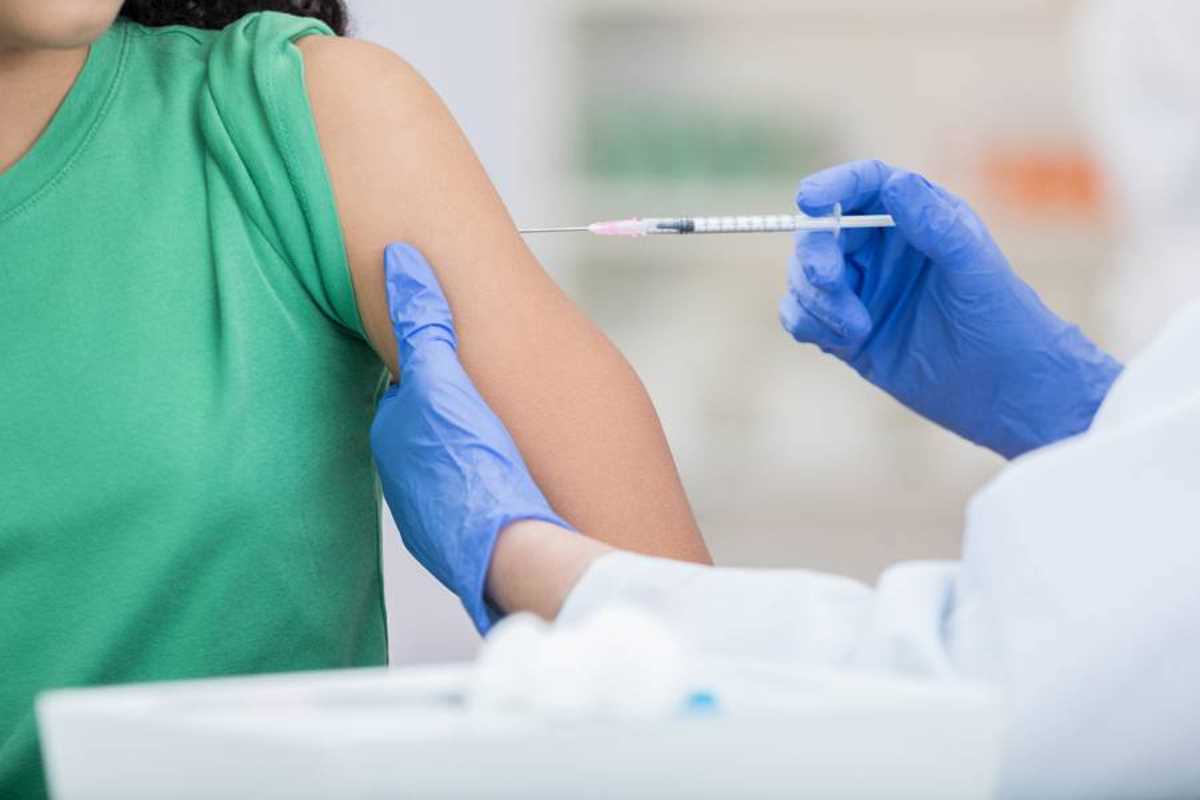
Each year, HPV causes more than 33,000 cases of cancers, including more than 90% of cervical cancers, as well as cancers of the vagina, vulva, penis, anus, and the area in the back of the throat called the oropharynx, according to the Centers for Disease Control and Prevention (CDC).
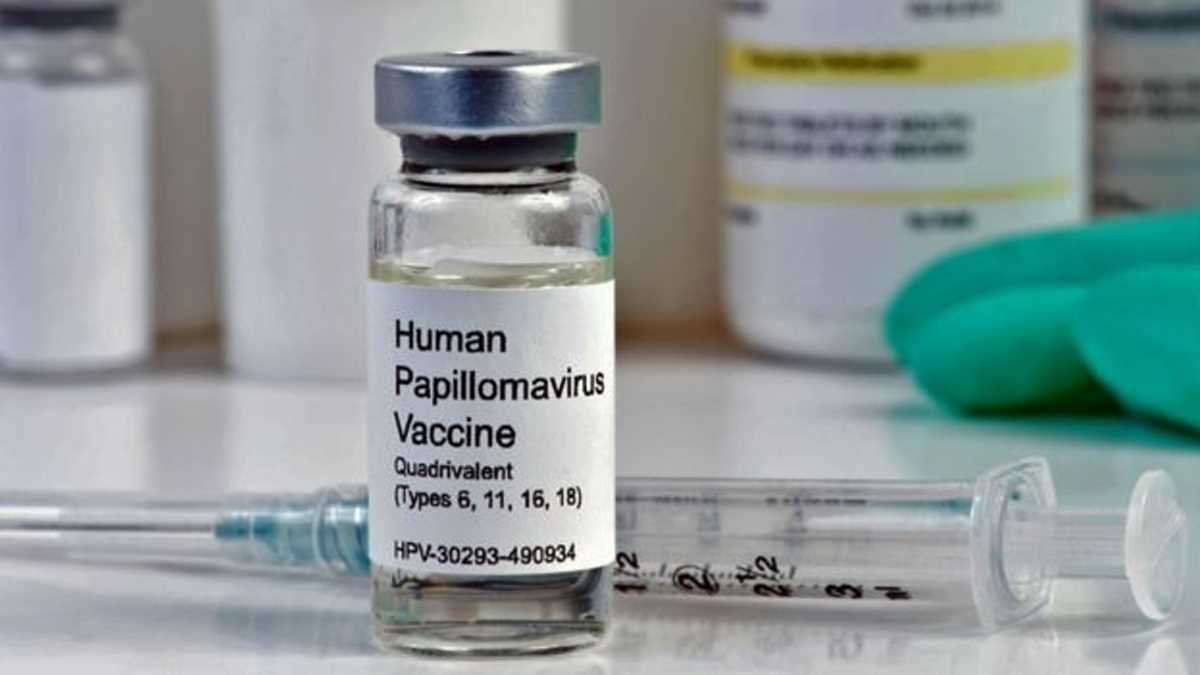
More than 40 types of HPV affect the genital area. Gardasil 9, the vaccine used in the United States, produced by the Merck laboratory, provides protection against nine of them, which together are associated with most HPV-related cancers and cause 90% of genital warts.
Because HPV is so common among sexually active people, the best time to get vaccinated is before sexual life begins and they are at risk of exposure to the virus. CDC’s Advisory Committee on Immunization Practices (ACIP) recommends HPV vaccination for all girls and boys ages 11 and 12. Catch-up vaccines for young people outside that age window are recommended up to age 21 for men and 26 for women (the proposed HPV vaccine update would change the vaccination guideline for men to align it with the 26-year limit for women).
At its June meeting, the immunization committee, made up of public health experts, recommended expanding the vaccination window to include adults between the ages of 27 and 45.
But instead of approving everyone in that age group, the panel said people should “make shared clinical decisions” with the health professional to determine if the vaccine is right for them.
“The ACIP made this kind of recommendation because most people in this age group are not likely to benefit from the vaccine,” CDC spokeswoman Kristen Nordlund wrote in an e-mail.
The vaccine will not protect people against the types of HPV to which they have already been exposed, and many sexually active people have been exposed to at least some types of HPV by age 20.
That makes it harder for the vaccine to impact this age group. A study of economic models presented at the ACIP meeting indicates that, according to current guidelines recommending immunization up to age 26, 202 people would have to be vaccinated to prevent one case of HPV-related cancer. When recommendations are expanded to include people up to 45, the number that would have to be vaccinated to prevent a cancer case increases exponentially to 6,500.
However, it is unlikely that people in the older age group were exposed to the nine types of HPV that the vaccine protects against.
“There is a sense that some protection can be obtained against some future cancers,” said Dr. William Schaffner, professor of preventive medicine and infectious diseases at Vanderbilt University School of Medicine, who is ACIP’s liaison for the National Foundation for Infectious Diseases.
However, patients, and their doctors, would have difficulty knowing if immunization would be beneficial.
“The problem is that no individual is likely to know what specific type of HPV he or she has been exposed to,” said Dr. Christopher Zahn, vice president of office activities at the American College of Obstetricians and Gynecologists.
Vaccine experts have some suggestions as to which people over the age of 26 might consider receiving the three-shot series. They include people with multiple sexual partners and those who are newly single and dating after being in a monogamous marriage or relationship.
Jennifer Sienko, 40, is in a better position than most people to evaluate whether or not to receive the vaccine. She is co-director of the National HPV Vaccination Roundtable, a coalition of HPV cancer reduction groups organized by the American Cancer Society.
But she was recently surprised when a new doctor asked if she wanted the vaccine. She said no.
Sienko, who lives in Chicago, has been married to her second husband for three years, and that weighed on her decision. But she said it might have been different when she was single for a while.
“There may have been a window where, if the vaccine had been indicated for older women, perhaps between my marriages, I would have investigated the possibility,” she said.
The CDC is reviewing the ACIP recommendation. If it passes, experts hope the CDC will provide more guidance in determining who the vaccine is appropriate for.
If the CDC approves extending the age of the vaccine in consultation with a health-care provider, most insurers would cover the costs — a few hundred dollars per dose. Under the preventive coverage rules of the Affordable Care Act (ACA), patients generally won’t have to pay anything out of pocket.